Medicine That Transforms – Boston Health Care for the Homeless Program
Lisa Leslie Henderson writer
Photography Courtesy of Boston Health Care for the Homeless Program
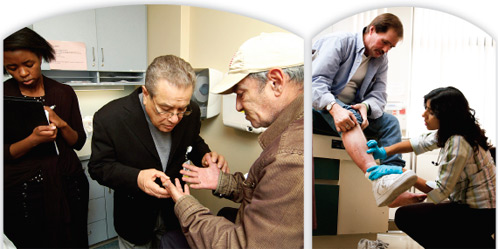
It has been another ten-hour day for Gretchen Treves, the fourth one this week. “A long, but satisfying day,” she concluded as she drove home to Weston from the respite care center at Boston Health Care for the Homeless Program (BHCHP) where she works as a Physician Assistant. Several familiar faces on rounds this morning and a handful of smiles conveying recognition and gratitude made the difference between a long, exhausting day and a long but satisfying workday. Being able to tag on some overdue preventive care while tending to her patient’s acute medical needs reminded her of why she had left emergency medicine to join the 200 medical professionals at BHCHP, whose mission is to provide or assure access to the highest quality health care for all homeless men, women, and children in the greater Boston area.
“As trite as it may sound, I wanted to be able to make a difference,” explains Treves. “Our clients are some of the city’s most vulnerable people; patients who really need medical care and often have a hard time accessing it.”
What Treves and her colleagues are doing at BHCHP is anything but trite. Years of living on the streets and in shelters have taken their toll on their patients, whose forty-year-old bodies often resemble those of sixty-year-olds. Most live with multiple illnesses and, as a result of childhood trauma, battle addiction, mental illness, or both. It’s quite a load for anyone to carry, and it has become especially challenging over the last decade, as an emphasis on shortened hospital stays has made home-based recovery essential. BHCHP provides an answer to the question raised by this paradigm shift: Where does one recover if one doesn’t have a home?
 Ross, Janice, and George are typical of Treves’ patients. BHCHP personnel have been working with Ross, a diabetic, to manage his blood sugar levels. They’ve experimented with various doses and types of insulin to compensate for the fact that he can’t keep it refrigerated. They’ve negotiated with a local shelter to provide access to syringes to administer the insulin, as possession of needles can be grounds for being denied a bed. In spite of everyone’s best efforts, Ross had been admitted the night before with a dangerously high blood sugar level, which Treves’ team had successfully brought under control. They were also able to tend to his trench foot, a medical condition commonly seen in the trenches of the First World War and now among many homeless people, caused by prolonged exposure to damp or unsanitary conditions. Left untreated, gangrene could set in, leading to potential amputation.
Ross, Janice, and George are typical of Treves’ patients. BHCHP personnel have been working with Ross, a diabetic, to manage his blood sugar levels. They’ve experimented with various doses and types of insulin to compensate for the fact that he can’t keep it refrigerated. They’ve negotiated with a local shelter to provide access to syringes to administer the insulin, as possession of needles can be grounds for being denied a bed. In spite of everyone’s best efforts, Ross had been admitted the night before with a dangerously high blood sugar level, which Treves’ team had successfully brought under control. They were also able to tend to his trench foot, a medical condition commonly seen in the trenches of the First World War and now among many homeless people, caused by prolonged exposure to damp or unsanitary conditions. Left untreated, gangrene could set in, leading to potential amputation.
Just down the hall rests Janice, who is slowly recovering from a sexual assault earlier in the week—an all-too-common experience of homeless women, and this one combined with a blow to the head. Treves secured a consultation with a BHCHP psychiatrist and scheduled a mammogram for her today—little steps, but steps that say, “You matter.”

“As trite as it may sound, I wanted to be able to make a difference.”
– Gretchen Treves
George had been in residence for just over a week, having been referred by a local hospital to BHCHP following open-heart surgery. He was quite sore and his ribs still needed to heal, but more acute cases were being admitted and he was technically well enough to be released. Case managers had worked very hard to arrange stable housing for George so that he would not have to return to the street.
“We’re closing a crucial gap,” explains Treves. “Without BHCHP, many of these people would be left untreated or would have no alternative to expensive emergency room treatment and extended hospital stays.” In so doing, BHCHP is breathing life into some of Boston’s most discouraged and destitute persons while simultaneously decreasing the cost of care for some of the city’s most expensive patients.
How is it possible that by providing increased medical care to Boston’s 11,000-plus homeless people, BHCHP is actually containing health care costs? Wellesley’s Margaret Boles Fitzgerald, a long-time BHCHP board member and now its Director of Corporate and Foundation Relations, will tell you that the secret is in proactively providing top-notch medical care in a variety of cost-effective settings. BHCHP’s $33 million operating budget funds approximately 100,000 such “health encounters” annually. These interactions help to avoid health care emergencies, debilitating illnesses, and even premature fatalities (Boston’s chronically homeless typically die in their late forties), all of which incur tremendous human and financial costs.
 The obstacles to wellness can be overwhelming for many of us, but are especially formidable for this unique population. Homelessness is frighteningly chaotic. Basics like eating right, getting enough rest and exercise, reducing stress, and keeping track of medications pose tremendous challenges for those who don’t have a place to call home. Violence and extreme conditions are commonplace on the streets, as is exposure to a variety of communicable diseases in crowded shelters. Making an effort to see a doctor — who will accept their insurance, speak their language, and understand the context of their illness and ability to recover — is not high on the list of priorities for people who are not sure where their next meal will come from, who begin lining up to secure a bed in local shelters daily at 3:00 pm, and whose addiction or mental illness may lead them to believe that they aren’t even sick.
The obstacles to wellness can be overwhelming for many of us, but are especially formidable for this unique population. Homelessness is frighteningly chaotic. Basics like eating right, getting enough rest and exercise, reducing stress, and keeping track of medications pose tremendous challenges for those who don’t have a place to call home. Violence and extreme conditions are commonplace on the streets, as is exposure to a variety of communicable diseases in crowded shelters. Making an effort to see a doctor — who will accept their insurance, speak their language, and understand the context of their illness and ability to recover — is not high on the list of priorities for people who are not sure where their next meal will come from, who begin lining up to secure a bed in local shelters daily at 3:00 pm, and whose addiction or mental illness may lead them to believe that they aren’t even sick.
Although patients who are chronically homeless generally have preventable or curable diagnoses—asthma, diabetes, gastrointestinal disorders, hypertension, pneumonia, and tuberculosis—they often go untreated. As a result, curable illnesses often morph into advanced medical conditions that are expensive to treat. Addiction and mental illness add further complexity to the landscape.
“BHCHP is successful because it has reinvented health care delivery to this quite vulnerable population,” Margaret Boles Fitzgerald says.
As a result of its extensive partnerships with local institutions, BHCHP is able to provide medical care to its clients where they are, within the context of their lives. Medical personnel are available in over 80 locations including soup kitchens, shelters, and two hospital-based clinics located at either end of the city. A Street Outreach Team reaches out to “rough sleepers”—those who cannot tolerate homeless shelters or mainstream clinics and hospitals—making house calls in alleyways, under bridges, and near heated grates. Multiple local institutions make referrals to BHCHP’s respite care center, allowing the healing process to take hold. Such effective partnering eliminates duplication of services, enhancing the efficiency of Boston’s safety net.
Another factor in BHCHP’s success is its integrated approach to healing, which combines primary care, behavioral health, and dental care all in one setting. Case managers augment these resources, helping patients to apply for benefits, secure spots in detox and rehabilitation programs, identify housing and training opportunities, and coordinate their care. Electronic medical records that follow patients from street to clinic, to hospitals, to respite care, to shelters, and, for the lucky ones, to more permanent housing, assure that each of BHCHP’s patients are known to every BHCHP team member, providing a consistency and continuity that is missing in homeless persons’ lives and a critical ingredient for effective ongoing treatment.
 More important than where and what services are provided, however, is how BHCHP provides care. Respect and dignity are hallmarks of BHCHP’s care. Unlike many programs created for temporarily homeless persons that reward people for successfully meeting certain milestones, BHCHP understands the revolving door nature of mental illness and addiction that is often a characteristic of the chronically homeless. They practice tough love, but with an understanding of the all-consuming circumstances in which their patients live.
More important than where and what services are provided, however, is how BHCHP provides care. Respect and dignity are hallmarks of BHCHP’s care. Unlike many programs created for temporarily homeless persons that reward people for successfully meeting certain milestones, BHCHP understands the revolving door nature of mental illness and addiction that is often a characteristic of the chronically homeless. They practice tough love, but with an understanding of the all-consuming circumstances in which their patients live.
“It’s really, really hard being homeless,” says Treves. ”Trying to manage a disease without having the basic things in life that we take for granted, like a safe place to live and a secure place to keep your personal items, is incredibly difficult.”
Many BHCHP patients do get better, but it is hard for them to lead more productive lives as long as they remain homeless, and alone, without the social support network that we all need to succeed in life.
“One of our doctors talks about how she wishes that she could write a prescription for housing along with medicine,” Boles Fitzgerald says. Research shows that health care costs for individuals go down substantially when they become housed; unfortunately, affordable housing is limited in the Boston area, and it takes a great deal of support to make the transition from the street to a home successful.
 So why is it that talented people like Treves and Boles Fitzgerald are willing to put in the hours for work that can be Sisyphean in nature? For starters, the jobs at BHCHP are fascinating and require some of the best medical minds out there. Not surprisingly, many of BHCHP physicians and dentists are on the teaching faculty of Harvard, Boston University, and Tufts, and their groundbreaking work is being replicated throughout the country.
So why is it that talented people like Treves and Boles Fitzgerald are willing to put in the hours for work that can be Sisyphean in nature? For starters, the jobs at BHCHP are fascinating and require some of the best medical minds out there. Not surprisingly, many of BHCHP physicians and dentists are on the teaching faculty of Harvard, Boston University, and Tufts, and their groundbreaking work is being replicated throughout the country.
Working at BHCHP can also be deeply satisfying. “It is a privilege to be able to reduce someone’s pain, to take a stab at restoring their health, or rekindle a bit of hope in their lives,” explains Treves.
While it may seem obvious who is giving and who is receiving at BHCHP, both Treves and Boles Fitzgerald will tell you that it is not always clear who gets more from these relationships: BHCHP employees or the patients.
“Transformation takes place every day here, in everyone’s life,” Boles Fitzgerald explains. “My colleagues are teaching me to truly look at our patients through a lens of worth and dignity; it’s a lesson in love dispensed without the jaundiced eye of prejudice or ignorance. By working alongside them, I am becoming more of the person I want to be.”
Treves explains this transformation: “Once you begin to get to know our patients as individuals, rather than as a category, your heart begins to open—you begin to soften. Through listening to their stories, you realize that anyone who is ‘human’ enough to make mistakes, or have an issue that may affect their ability to make a living, could find themselves homeless. It’s quite humbling.”
In this way, BHCHP makes a difference, simultaneously transforming its patients, providers, administrators, and Boston’s health care delivery system, one health encounter at a time. ![]()
Be a Part of the Difference

© 2011 Elm Bank Media | Beth Furman, Publisher | Beth@ElmBankMedia.com


recent comments